Fraud Detection Practices: What Your Benefits Data Might Not Show
Reveal unseen fraud, waste and abuse in your benefits data and know how HR teams can stay in control.
Reveal unseen fraud, waste and abuse in your benefits data and know how HR teams can stay in control.

While your medical benefits are designed to keep you healthy, they are not to be overused. Seemingly harmless habits could count as fraud, waste, or abuse (FWA).
What is FWA?
Excessive or fraudulent claims will eventually drive up overall utilisation, leading to higher insurance premiums, renewal costs, and reduced negotiating power with providers.
As costs increase, organisations may be forced to cut coverage, lower limits, or tighten policies, affecting the value of benefits for the broader workforce.
Fraudulent claims and unnecessary medical leave can contribute to absenteeism, workflow disruptions, and heavier workloads for other team members.
When claims data is inflated by misuse or abuse, HR may make inaccurate decisions around benefit design, provider partnerships, and budget allocation.

Seeing that FWA could negatively affect the organisation, there is even more a need to manage its root causes. While it cannot be totally removed, efforts can be made to reduce such events.
A HR professional’s most powerful tool is the organisation’s first-hand data. This includes attendance, leave, and claims records. Here are some best practices used by data-driven organisations.
In this first practice, you might want to spot anomalies in your claims records. Consider these patterns:
Though these situations are far from ideal, they can make way for honest conversations with employees for interventions and improvements down the line.
Monitoring such data will lead to much more informed decisions, enabling organisations to take proactive corrective action.
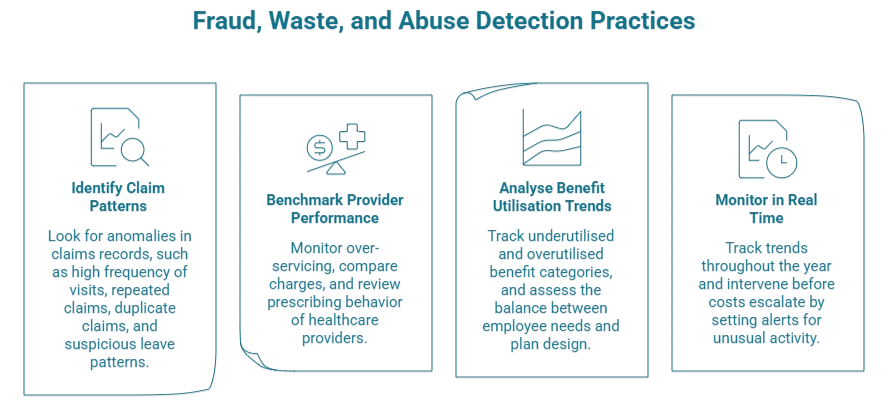
When fraud, waste or abuse is detected, organisations can work to review irregular charges or prescribing behaviour, strengthen policy controls, and educate employees on responsible benefit utilisation. Even before issues arise, we want to take measures to safeguard against such events from happening from the get-go.
Technology can only do so much to detect fraudulent practices. Prevention, and the how or why employee benefits are utilised is reliant on the culture set at the workplace. This is where HR professionals are key in shedding light to employees on abuse vs genuine utilisation, communicating governance on such events, and reinforcing company values.
Collaborating with your fellow employees could encourage an anti-fraudulent work ethic. To start the conversation, share these following efforts that everyone can be a part of, as well as HR-specific considerations.
Another way to prevent FWA is to consider partnering with a platform with analytics capabilities, real-time reports, and health provider benchmarks. Perhaps here are some questions to ask your potential benefits partner.
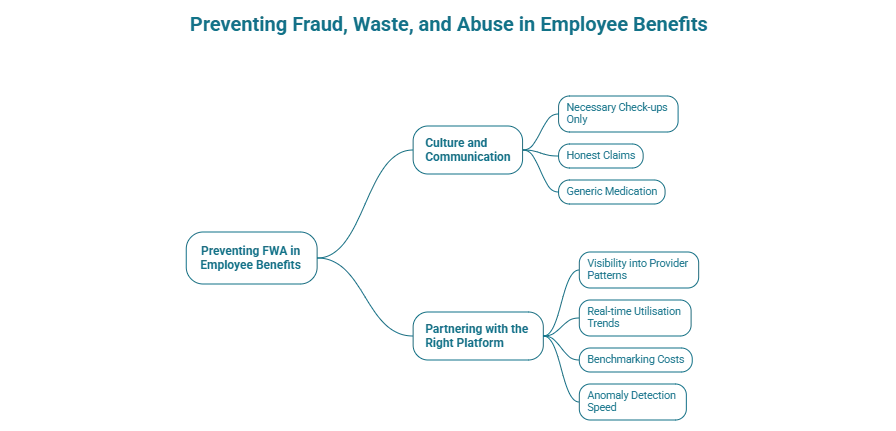
Bringing it altogether, it matters to detect through data and analytics, prevent through policies and controls, and optimise with revised employee benefits plan(s). Fraud, waste and abuse don’t arrive as a crisis. They accumulate quietly, claim by claim. The organisations that win are the ones that spot the pattern before it becomes a problem. Let’s figure it out together!

HealthMetrics is a unified digital TPA platform designed to streamline healthcare administration for insurers and corporates across Southeast Asia. It connects you to a regional healthcare network, automates claims and benefit management, and delivers real-time insights to optimise cost, care, and experience.
Whether you’re managing members at scale or navigating complex cross-border care, HealthMetrics empowers you with smarter tools and a seamless ecosystem.
Explore the HealthMetrics Platform or connect with our team to learn how we’re transforming healthcare access.
48 hours saved in benefit reimbursement.
HealthMetrics’ data-driven approach has been able to accelerate the processing of employee's health benefits significantly.
Read study >
85% reduction in administrative task
Companies can reduce up to 85% of time spent on HR administrative task and this frees up time for HR on more important tasks.
Read study >
Our pricing plans vary in terms of the features and services that are included, so you can select the one that offers the right mix of benefits for your specific requirements. Whether you are a small business owner, a freelancer, or a larger organisation, we have a pricing plan that is tailored to your needs.
You can view the details of each pricing plan on our website, and our customer support team is always available to answer any questions you may have and help you choose the right one for you.
Reach out to our 24/7 customer support through multiple channels.